This article explains the different types of thalassemia, focusing on alpha and beta thalassemia. It helps patients and families understand how these genetic blood disorders differ in causes, severity, and symptoms. The guide also provides simple insights into diagnosis and management, making it easier for readers to recognize and manage thalassemia effectively.
Types of Thalassemia: The Genetic Basis of Thalassemia
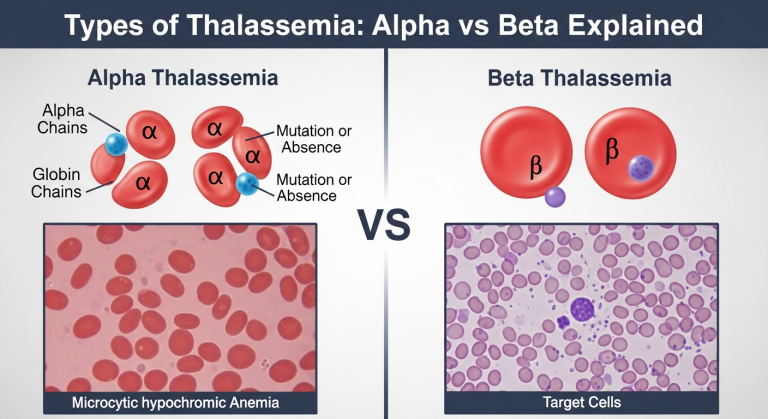
To understand thalassemia, you first need to understand how the body produces hemoglobin. Hemoglobin is a complex protein made of two main parts: alpha globin chains and beta globin chains. You can think of these chains as building blocks. A healthy red blood cell needs a perfectly balanced number of alpha and beta blocks to function properly and carry oxygen effectively.
Your genes dictate how these blocks are made. You inherit these genes from your parents. If there is a mutation or a deletion in the genes responsible for creating either the alpha or the beta chains, the body cannot produce enough of that specific block.
When this genetic error occurs, the red blood cells do not form correctly. They become smaller, paler, and less capable of transporting oxygen. Furthermore, the imbalance between the alpha and beta chains causes the red blood cells to break down faster than normal. This rapid destruction of red blood cells results in anemia, leaving the person feeling constantly tired and weak.
Types of Thalassemia: Alpha Thalassemia – A Closer Look
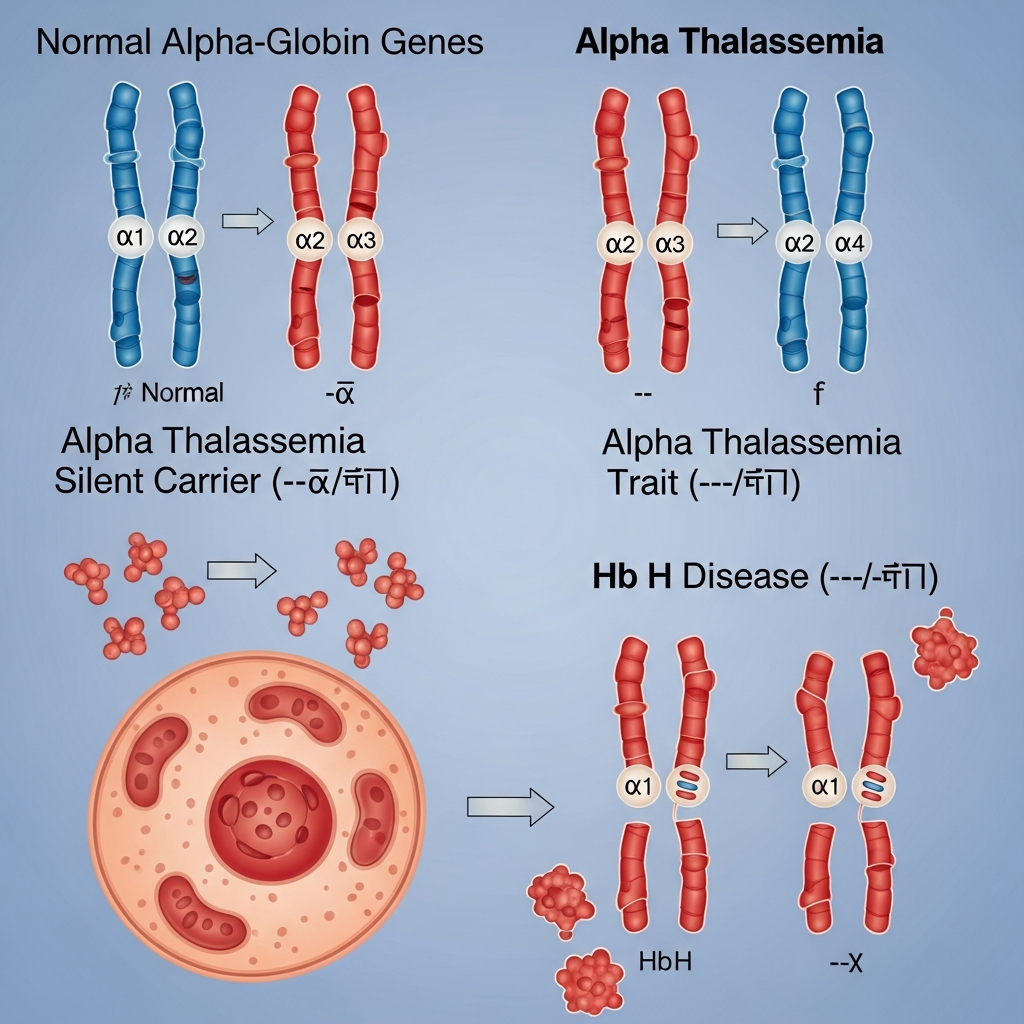 Alpha thalassemia occurs when there is a problem with the genes that produce the alpha globin chains. Humans normally have four genes responsible for making alpha globin, inheriting two from each parent. The severity of alpha thalassemia depends directly on how many of these four genes are missing or mutated.
Alpha thalassemia occurs when there is a problem with the genes that produce the alpha globin chains. Humans normally have four genes responsible for making alpha globin, inheriting two from each parent. The severity of alpha thalassemia depends directly on how many of these four genes are missing or mutated.
This section of types of thalassemia focuses on the different clinical forms of alpha thalassemia based on gene loss.
The Four Degrees of Alpha Thalassemia
1. Silent Carrier State
When only one of the four genes is missing or altered, the person is a silent carrier. People in this category usually have no symptoms. Their hemoglobin levels remain normal, and they are generally healthy. However, they can still pass the mutated gene to their children.
2. Alpha Thalassemia Trait
If two genes are missing, the individual has alpha thalassemia trait. This may cause very mild anemia. It is often discovered accidentally during routine blood tests, where red blood cells appear slightly smaller than normal. No specific treatment is usually required.
3. Hemoglobin H Disease
When three genes are missing, the condition becomes Hemoglobin H disease. This leads to moderate to severe anemia because excess beta chains form abnormal clusters called Hemoglobin H. These damage red blood cells and cause symptoms such as fatigue, jaundice, enlarged spleen, and bone changes. Ongoing medical care and sometimes blood transfusions are needed.
4. Hydrops Fetalis (Alpha Thalassemia Major)
When all four genes are missing, it results in the most severe form. The fetus cannot produce functional hemoglobin, leading to life-threatening complications. Most cases result in stillbirth or death shortly after birth. Rarely, early diagnosis and in-utero transfusions may improve survival.
Types of Alpha Thalassemia at a Glance (Table)
| Type |
Number of Genes Affected |
Severity |
Symptoms |
Treatment Need |
| Silent Carrier |
1 gene |
Very mild / none |
Usually no symptoms |
None |
| Alpha Thalassemia Trait |
2 genes |
Mild |
Slight anemia, small red blood cells |
Usually none |
| Hemoglobin H Disease |
3 genes |
Moderate to severe |
Anemia, fatigue, jaundice, enlarged spleen |
Regular care, possible transfusions |
| Hydrops Fetalis |
4 genes |
Life-threatening |
Severe fetal anemia, usually fatal |
Intensive prenatal intervention (rare cases) |
Key Points About Types of Thalassemia (Alpha Form)
- Severity increases as more alpha globin genes are missing.
- Many carriers show no symptoms but can pass the gene to offspring.
- The condition ranges from silent carrier state to life-threatening fetal disease.
- Early diagnosis is important for family planning and management.
- Genetic counseling is strongly recommended for affected families.
Geographic Distribution
Alpha thalassemia is most commonly found in populations from Southeast Asia, Southern China, the Middle East, and Africa. Its higher frequency in these regions is partly due to a genetic advantage: carrying one mutation can offer some protection against malaria, which is historically common in these areas.
Beta Thalassemia: A Comprehensive Overview
 Beta thalassemia happens when the genes responsible for producing beta globin chains are mutated. Unlike alpha globin, which uses four genes, beta globin production relies on only two genes—one inherited from each parent. The severity of beta thalassemia depends on whether one or both of these genes are faulty, and the extent of the mutation.
Beta thalassemia happens when the genes responsible for producing beta globin chains are mutated. Unlike alpha globin, which uses four genes, beta globin production relies on only two genes—one inherited from each parent. The severity of beta thalassemia depends on whether one or both of these genes are faulty, and the extent of the mutation.
The Three Main Types of Beta Thalassemia
Beta Thalassemia Minor
Also known as the beta thalassemia trait, this occurs when one of the two beta genes is mutated while the other functions normally. People with beta thalassemia minor usually experience no serious symptoms. They might have mild anemia that is sometimes misdiagnosed as an iron deficiency. Like the alpha silent carriers, they live normal lives but can pass the gene to their children.
Beta Thalassemia Intermedia
When both genes are mutated, but the body can still produce a small amount of functional beta globin, the condition is called beta thalassemia intermedia. The symptoms range from moderate to severe. Some patients manage well with occasional medical interventions, while others might develop bone abnormalities, an enlarged spleen, and a need for infrequent blood transfusions.
Beta Thalassemia Major (Cooley’s Anemia)
This is the most severe form of beta thalassemia. It occurs when both beta genes are completely non-functional. Babies born with Cooley’s anemia usually appear healthy at birth but develop severe, life-threatening anemia within their first two years of life. Symptoms include poor growth, skeletal deformities, and severe fatigue. People with beta thalassemia major require lifelong, frequent blood transfusions to survive.
Geographic Distribution
Beta thalassemia is highly prevalent in Mediterranean countries, such as Greece and Italy. It is also quite common in parts of the Middle East, Central Asia, and the Indian subcontinent. Similar to the alpha variant, the genetic trait survived in these populations due to the protection it provided against malaria.
Types of Thalassemia: Differentiating Alpha and Beta Thalassemia
While both alpha thalassemia and beta thalassemia affect the blood and share similar symptoms like fatigue and anemia, they are fundamentally different at the genetic level. Understanding this difference is an important part of learning the types of thalassemia, especially for accurate diagnosis and management.
Key Genetic Differences
The main difference lies in the genes and chromosomes involved:
- Alpha thalassemia affects the alpha globin genes located on chromosome 16. There are four genes involved (two from each parent).
- Beta thalassemia affects the beta globin genes located on chromosome 11, and there are only two genes (one from each parent).
Because of this structural difference, the way the disease develops and its severity patterns are not the same.
Clinical Differences Between Alpha and Beta Thalassemia
1. Severity at Birth and Disease Progression
- Alpha thalassemia (severe form – Hydrops Fetalis):
- Often causes death before or shortly after birth.
- The fetus cannot produce functional hemoglobin at all.
- Beta thalassemia (severe form – Cooley’s anemia / beta thalassemia major):
- Babies are usually born without major visible issues.
- Symptoms develop gradually within the first 6–24 months of life.
2. Symptoms Comparison
| Feature |
Alpha Thalassemia |
Beta Thalassemia |
| Onset of symptoms |
In severe cases: before birth |
Usually after 6 months |
| Severity range |
Silent carrier → fatal fetal condition |
Mild trait → severe lifelong anemia |
| Major complications |
Hydrops fetalis (fatal in most cases) |
Growth delay, bone deformities, iron overload |
| Transfusion need |
Only in Hemoglobin H disease |
Regular in major form |
3. Disease Pattern
- Alpha thalassemia: Severity depends on how many of the four genes are missing.
- Beta thalassemia: Severity depends on whether mutations affect one or both genes.
Diagnosis: How Doctors Differentiate Them
Doctors use a step-by-step approach to identify the exact type of thalassemia:
1. Complete Blood Count (CBC)
- Measures hemoglobin level
- Shows red blood cell size and shape
- Suggests presence of anemia but not the exact type
2. Hemoglobin Electrophoresis
- Separates and identifies different types of hemoglobin
- Helps distinguish alpha thalassemia vs beta thalassemia
- Especially useful for detecting abnormal hemoglobin patterns in beta thalassemia
3. Genetic (DNA) Testing
- Most accurate method
- Identifies exact gene deletions or mutations
- Confirms diagnosis and helps with family planning
Key Takeaways in Types of Thalassemia
- Alpha and beta thalassemia affect different genes and chromosomes.
- Alpha thalassemia can be more severe before birth, while beta thalassemia often shows symptoms after infancy.
- Both conditions require different diagnostic tools for confirmation.
- Genetic testing is the most reliable method for accurate classification.
- Early detection helps in better management and genetic counseling.
Living with Thalassemia: Challenges and Support
 Living with a severe form of thalassemia heavily impacts a person’s daily life. The disorder demands rigorous, ongoing medical management.
Living with a severe form of thalassemia heavily impacts a person’s daily life. The disorder demands rigorous, ongoing medical management.
For many patients, the foundation of treatment involves regular blood transfusions, often every two to four weeks. These transfusions keep hemoglobin at a safe level. However, frequent blood transfusions create a new, dangerous problem: iron overload. The human body does not have a natural way to get rid of excess iron. Over time, the iron from the transfused blood builds up in the heart, liver, and endocrine system, causing fatal organ damage.
To combat this, patients must undergo chelation therapy. Chelation involves taking specific medications that bind to the extra iron in the body and help excrete it through urine or stool. This daily medication is an absolute necessity for survival.
Currently, the only potential cure for thalassemia is a bone marrow transplant, also known as a stem cell transplant. This procedure replaces the patient’s faulty blood-forming stem cells with healthy ones from a matching donor, usually a sibling. However, the procedure carries severe risks and requires a perfectly matched donor, making it unavailable for many patients.
Genetic counseling plays a massive role in managing the disease on a community level. Because thalassemia is entirely genetic, carriers must understand the risks of passing the condition to their children. If two carriers of the beta thalassemia trait have a child, there is a 25% chance the baby will have beta thalassemia major.
Patient advocacy groups and support networks are vital. Dealing with a chronic, life-long illness can be emotionally and financially draining. Support groups provide families with shared experiences, mental health resources, and guidance on navigating complex medical systems.
Types of Thalassemia: Research and Future Directions
The future holds incredible promise for people affected by types of thalassemia. Medical research is advancing rapidly, offering hope for more effective treatments and, in some cases, long-term cures.
Gene Therapy and Genetic Editing
Advances in gene therapy are at the forefront of thalassemia research. Scientists are working on innovative methods to correct the underlying genetic defect rather than just treating symptoms.
The process generally involves:
- Collecting the patient’s own stem cells
- Using gene-editing tools like CRISPR to correct the faulty hemoglobin gene in a laboratory
- Infusing the repaired cells back into the patient’s body
Early clinical trials have shown very promising results. For some patients, this approach may significantly reduce or even eliminate the need for lifelong blood transfusions. This marks a major shift in the future management of types of thalassemia.
New Drug Developments
Alongside gene therapy, researchers are developing new medications that improve how the body produces and uses red blood cells.
These newer treatments aim to:
- Increase the production of healthy hemoglobin
- Help red blood cells mature more effectively
- Reduce the frequency of blood transfusions
- Improve overall energy levels and quality of life
Some recently approved drugs are already showing success in reducing transfusion dependence, especially in beta thalassemia patients.
Early Detection and Prevention
Prevention remains one of the most powerful tools in reducing the burden of types of thalassemia worldwide.
Modern strategies include:
- Widespread carrier screening programs in high-risk regions
- Genetic counseling for couples planning to have children
- Prenatal testing to detect severe forms early in pregnancy
- Public awareness campaigns about inherited blood disorders
By identifying carriers early, families can make informed decisions and reduce the chance of passing on severe forms of the disease.
Moving Forward with Hope
Thalassemia is a complex genetic condition that affects hemoglobin production due to defects in globin genes. Whether it is alpha thalassemia involving four genes on chromosome 16 or beta thalassemia involving two genes on chromosome 11, the result is the same: impaired oxygen transport in the body.
While severe forms require ongoing medical care such as blood transfusions and iron chelation therapy, the treatment landscape is improving rapidly. Gene editing, advanced drug therapies, and improved screening programs are transforming what was once a life-limiting condition into one with far greater hope.
Final Key Points
- Types of thalassemia research is rapidly evolving, especially in gene therapy
- CRISPR-based treatments may offer long-term correction in the future
- New drugs are reducing dependence on blood transfusions
- Early screening and genetic counseling help prevent severe cases
- Awareness and research funding are essential for continued progress
Frequently Asked Questions
1. What are the main types of thalassemia?
The main types of thalassemia are alpha thalassemia and beta thalassemia. Both affect hemoglobin production but involve different genes and chromosomes. Understanding these is essential when studying the types of thalassemia.
2. What causes thalassemia?
Thalassemia is caused by genetic mutations or deletions in the genes responsible for producing hemoglobin chains (alpha or beta globin). It is inherited from parents and is a key part of the types of thalassemia classification.
3. Is thalassemia contagious?
No, thalassemia is not contagious. It is a genetic condition passed from parents to children through inherited genes and is included under the types of thalassemia disorders.
4. What is the difference between alpha and beta thalassemia?
Alpha thalassemia involves four genes on chromosome 16, while beta thalassemia involves two genes on chromosome 11. They also differ in severity and symptoms, making them two major categories in types of thalassemia.
5. Can a person have mild thalassemia?
Yes. Many people with thalassemia trait or silent carrier states have mild or no symptoms and may not even know they have the condition. These mild forms are part of the broader types of thalassemia spectrum.
6. What are common symptoms of thalassemia?
Common symptoms include fatigue, weakness, pale skin, slow growth in children, and in severe cases, bone deformities and enlarged spleen. Symptoms vary depending on the types of thalassemia.
7. How is thalassemia diagnosed?
Doctors use blood tests like CBC, hemoglobin electrophoresis, and genetic testing to identify the type and severity of thalassemia. These tests help determine the exact types of thalassemia a patient may have.
8. Can thalassemia be cured?
Currently, the only potential cure is bone marrow or stem cell transplantation. However, gene therapy is emerging as a promising future treatment for different types of thalassemia.
9. What is the most severe form of thalassemia?
In alpha thalassemia, the most severe form is hydrops fetalis. In beta thalassemia, it is beta thalassemia major (Cooley’s anemia). These are critical conditions within types of thalassemia.
10. Can thalassemia be prevented?
While it cannot be fully prevented, genetic screening and counseling can help reduce the risk of passing severe forms to children. Prevention strategies are important in managing types of thalassemia globally.
Conclusion
If you or a loved one has a family history of blood disorders, a simple blood test and genetic consultation can provide clarity. With continued research, education, and global awareness, the future for people living with types of thalassemia is becoming increasingly hopeful, with the possibility of safer, more effective, and even curative treatments ahead.
 Beta thalassemia happens when the genes responsible for producing beta globin chains are mutated. Unlike alpha globin, which uses four genes, beta globin production relies on only two genes—one inherited from each parent. The severity of beta thalassemia depends on whether one or both of these genes are faulty, and the extent of the mutation.
Beta thalassemia happens when the genes responsible for producing beta globin chains are mutated. Unlike alpha globin, which uses four genes, beta globin production relies on only two genes—one inherited from each parent. The severity of beta thalassemia depends on whether one or both of these genes are faulty, and the extent of the mutation.