Anemia classification refers to the systematic categorization of anemia based on causes, red blood cell size, and severity. It helps healthcare professionals diagnose underlying conditions accurately and choose appropriate treatments for improved patient outcomes and better blood health management.
This inherited genetic disorder directly impacts the production of hemoglobin protein chains. Patients with this condition produce structurally abnormal hemoglobin, leading to small, easily destroyed red blood cells. Managing this condition requires specialized care and regular monitoring, which you can explore further in a comprehensive thalassemia awareness and management guide.
Etiological Anemia Classification (By Cause)
While morphological classification looks at the cells’ appearance, etiological anemia classification organizes the condition based on the underlying physiological cause. This approach answers the fundamental question of why the blood count is low.
Anemia due to Blood Loss
Losing blood is a direct and obvious way to deplete red blood cell counts. The medical approach changes entirely depending on how quickly the blood is lost.
Acute Hemorrhage
Sudden trauma, complications during childbirth, or a ruptured blood vessel can cause rapid blood volume depletion. The immediate medical priority is stopping the bleeding and restoring the body’s fluid volume to prevent shock.
Chronic Blood Loss
A slow, unnoticed leak over months or years eventually drains the body’s iron reserves. Gastrointestinal issues like ulcers, polyps, or colon cancer are frequent causes, as are heavy menstrual cycles. Identifying the source of the bleeding is paramount for long-term health.
Anemia due to Decreased Red Blood Cell Production
Sometimes the factory itself is the problem. If the bone marrow lacks the proper materials or instructions, it cannot keep up with the body’s demand for new blood cells.
Nutritional Deficiencies
A diet lacking in essential building blocks directly halts production. Iron, Vitamin B12, and folate are all strictly required for the creation of healthy red blood cells. Treating these deficiencies often resolves the symptoms entirely.
Bone Marrow Disorders
Diseases that directly damage the bone marrow severely limit blood cell creation. Aplastic anemia, myelodysplastic syndromes, and pure red cell aplasia replace or destroy the healthy stem cells required to sustain human life.
Kidney Disease
Healthy kidneys produce a hormone called erythropoietin, which acts as a chemical messenger telling the bone marrow to make more red blood cells. When the kidneys fail, erythropoietin levels plummet, and the bone marrow slows its production.
Chronic Inflammation
Systemic illnesses continuously release inflammatory proteins that interfere with iron metabolism and blunt the bone marrow’s response to erythropoietin, resulting in a steady decline in red blood cell counts.
Anemia due to Increased Red Blood Cell Destruction (Hemolytic Anemia)
Red blood cells typically live for about 120 days. Hemolytic conditions drastically shorten this lifespan, forcing the bone marrow to work overtime in a futile attempt to replace the dying cells.
Inherited Hemolytic Anemias
Many hemolytic conditions are passed down through genetics. Hemoglobinopathies, such as sickle cell disease and thalassemia, alter the structure of the cells, making them fragile. Fortunately, scientific advancements are changing the landscape for these inherited conditions, and you can learn more about these innovations by exploring gene therapy for thalassemia. Enzymopathies like G6PD deficiency remove the cell’s natural protections against oxidative stress, while membrane defects like hereditary spherocytosis cause the cells to lose their flexible shape.
Acquired Hemolytic Anemias
A person can be born with healthy red blood cells, only to have them destroyed by later medical developments. Autoimmune hemolytic conditions trick the body’s immune system into attacking its own blood cells. Certain medications can trigger drug-induced hemolysis. Microangiopathic conditions physically shred the cells as they pass through damaged blood vessels, and severe infections like malaria directly invade and rupture the red blood cells.
Advanced Anemia Classification Approaches
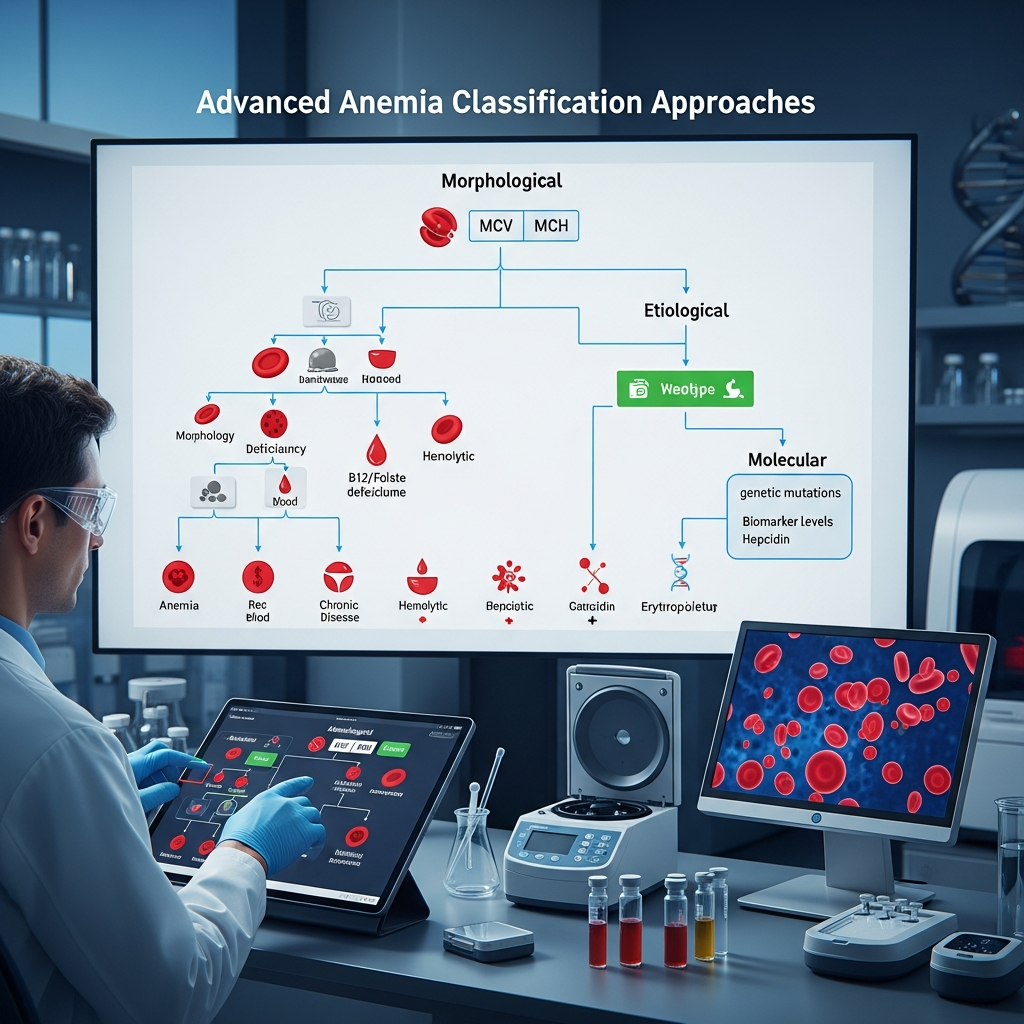 Modern medicine relies on a suite of sophisticated tests to classify anemia accurately. A standard Complete Blood Count (CBC) is just the beginning of the diagnostic journey.
Modern medicine relies on a suite of sophisticated tests to classify anemia accurately. A standard Complete Blood Count (CBC) is just the beginning of the diagnostic journey.
Red Blood Cell Indices
The CBC provides the MCV (Mean Corpuscular Volume), which measures cell size. It also delivers the MCH (Mean Corpuscular Hemoglobin), indicating the amount of hemoglobin per cell, and the MCHC (Mean Corpuscular Hemoglobin Concentration), showing the concentration of hemoglobin in a given volume of red blood cells. The RDW (Red Cell Distribution Width) measures the variation in cell size, helping doctors distinguish between mixed nutritional deficiencies and singular genetic traits.
Reticulocyte Count
Reticulocytes are immature red blood cells newly released from the bone marrow. Counting these young cells tells the doctor how hard the bone marrow is working. A high reticulocyte count indicates the marrow is functioning well and trying to replace lost or destroyed cells. A low count suggests the marrow is failing to produce cells, pointing toward a nutritional deficiency or bone marrow disorder.
Bone Marrow Examination
When blood tests cannot provide a definitive answer, doctors may perform a bone marrow biopsy. By extracting a small sample of the marrow tissue, usually from the hip bone, pathologists can look directly at the stem cells. This procedure is crucial for diagnosing aplastic anemia, leukemia, and other severe marrow disorders.
Molecular and Genetic Testing
For inherited blood disorders, looking at the DNA provides the ultimate confirmation. Genetic testing maps out the exact mutations causing conditions like sickle cell disease or thalassemia. This precise molecular classification helps predict disease severity and guides family planning decisions.
Clinical Significance of Accurate Anemia Classification
Categorizing blood disorders is not just an academic exercise. It is a critical clinical tool that dictates every step of the patient’s healthcare plan.
Guiding Diagnosis
Symptoms like fatigue and shortness of breath are incredibly vague. Proper classification narrows down a vast list of possible diseases to a manageable few. By determining if the cells are microcytic or macrocytic, doctors can skip unnecessary tests and zero in on the most likely culprit immediately.
Directing Treatment
Treatment protocols vary wildly depending on the classification. Prescribing iron pills for thalassemia or Vitamin B12 for acute blood loss is completely ineffective and potentially harmful. Finding an expert anemia treatment doctor ensures that the clinical data is interpreted correctly and that the prescribed therapy matches the specific physiological deficit.
Prognosis and Monitoring
Classification helps doctors predict the future course of the disease. A nutritional deficiency has an excellent prognosis with dietary changes. Conversely, a bone marrow failure requires aggressive, long-term interventions like stem cell transplants. Continuous monitoring based on the specific classification allows the medical team to adjust treatments as the patient’s body responds over time.
Moving Forward with Accurate Care
 Anemia classification is a complex but vital process that forms the backbone of effective hematological care. By evaluating the size, shape, and root causes of red blood cell deficiencies, medical professionals can solve the puzzle of chronic fatigue and oxygen deprivation.
Anemia classification is a complex but vital process that forms the backbone of effective hematological care. By evaluating the size, shape, and root causes of red blood cell deficiencies, medical professionals can solve the puzzle of chronic fatigue and oxygen deprivation.
If you are experiencing persistent exhaustion, pale skin, or unexplainable weakness, do not settle for guesswork. Seek a thorough medical evaluation. Demand a precise diagnosis that looks beyond the surface symptoms to uncover the exact nature of your blood health.


 One of the primary ways doctors categorize this blood condition is by examining the physical characteristics of the red blood cells under a microscope. This method, called morphological anemia classification, focuses heavily on the size of the cells. The Mean Corpuscular Volume (MCV) test provides this crucial measurement, dividing the condition into three main categories. This approach helps clinicians quickly narrow down potential causes and guide further diagnostic testing.
One of the primary ways doctors categorize this blood condition is by examining the physical characteristics of the red blood cells under a microscope. This method, called morphological anemia classification, focuses heavily on the size of the cells. The Mean Corpuscular Volume (MCV) test provides this crucial measurement, dividing the condition into three main categories. This approach helps clinicians quickly narrow down potential causes and guide further diagnostic testing. Certain conditions cause the red blood cells to grow large without the DNA synthesis issues seen in megaloblastic cases. Liver disease, chronic alcoholism, and specific bone marrow disorders like myelodysplastic syndromes frequently lead to the production of these large, non-megaloblastic cells. Proper anemia classification helps differentiate these causes for accurate treatment.
Certain conditions cause the red blood cells to grow large without the DNA synthesis issues seen in megaloblastic cases. Liver disease, chronic alcoholism, and specific bone marrow disorders like myelodysplastic syndromes frequently lead to the production of these large, non-megaloblastic cells. Proper anemia classification helps differentiate these causes for accurate treatment.