Learn about the beta thalassemia trait, including its genetic causes, possible symptoms, diagnosis methods, and why carrier testing is important for family planning and future health awareness. Discover how beta thalassemia trait is inherited, who should get tested, and what it means for children and future generations.
Blood health is a vital component of our overall well-being, yet many of us rarely think about the intricate details of our red blood cells unless an issue arises. Hemoglobin, the protein responsible for carrying oxygen throughout your body, relies on a delicate balance of alpha and beta chains. When there is a genetic variation affecting the production of these beta chains, it can lead to a condition known as the beta thalassemia trait.
Many individuals carry this genetic marker without ever realizing it. Because the trait usually causes no severe health problems, it can quietly pass from one generation to the next. People often discover their status only during routine blood work or when planning to start a family. Understanding your carrier status is incredibly important, as it provides crucial insight into your own health baseline and the potential genetic probabilities for your children.
Navigating genetic information can sometimes feel overwhelming, but gathering accurate facts empowers you to make informed medical decisions. By learning how this trait operates, how it is diagnosed, and what it means for your daily life, you can take a proactive approach to your health.
Understanding the Beta Thalassemia Trait
 The beta thalassemia trait, also referred to as beta thalassemia minor, occurs when a person inherits one mutated beta-globin gene and one normal beta-globin gene. This means the individual becomes a carrier of the condition rather than developing the severe form known as beta thalassemia major. People with the beta thalassemia trait often live completely healthy and normal lives without major medical complications.
The beta thalassemia trait, also referred to as beta thalassemia minor, occurs when a person inherits one mutated beta-globin gene and one normal beta-globin gene. This means the individual becomes a carrier of the condition rather than developing the severe form known as beta thalassemia major. People with the beta thalassemia trait often live completely healthy and normal lives without major medical complications.
This inherited blood disorder affects the body’s ability to produce normal hemoglobin, the protein in red blood cells responsible for carrying oxygen throughout the body. Because of this genetic mutation, red blood cells may become smaller than normal, which is why the condition is sometimes discovered during routine blood testing.
Understanding the beta thalassemia carrier state is important for family planning, genetic counseling, and early awareness. Many individuals do not realize they carry the trait until they undergo a thalassemia screening test or hemoglobin analysis.
How Genetics Play a Role
Genetics play a central role in the development of the beta thalassemia trait. Every person inherits two beta-globin genes, one from each parent. When only one gene carries a mutation, the person becomes a carrier and develops beta thalassemia minor rather than the severe disease.
According to the Centers for Disease Control and Prevention, this inherited condition is more common among people of Mediterranean, Middle Eastern, African, and Southeast Asian ancestry. In many regions, carrier screening programs help families understand their genetic risks before having children.
If two parents both carry the beta thalassemia trait, each pregnancy has:
- A 25% chance of producing a child with beta thalassemia major
- A 50% chance the child will inherit the carrier trait
- A 25% chance the child will inherit normal genes from both parents
Because of these risks, genetic counseling for thalassemia is highly recommended for couples with a family history of blood disorders or unexplained anemia.
Common Symptoms and Signs
For most individuals, the beta thalassemia trait causes no serious health problems. Many carriers remain completely asymptomatic throughout their lives and may only learn about the condition after a routine blood test or anemia screening.
In some cases, carriers can experience mild anemia symptoms such as:
- Slight fatigue or weakness
- Pale skin
- Mild dizziness
- Reduced energy levels
- Occasional shortness of breath during physical activity
These symptoms are usually mild because the body still produces enough healthy hemoglobin to function properly. Unlike severe thalassemia conditions, beta thalassemia minor rarely requires blood transfusions or intensive medical treatment.
However, mild anemia caused by the beta thalassemia carrier trait can sometimes be confused with iron deficiency anemia. This is why proper thalassemia testing, including hemoglobin electrophoresis and genetic testing, is essential for an accurate diagnosis. If you often feel unusually tired or notice persistent anemia symptoms, consulting a healthcare professional is strongly recommended.
Understanding the Beta Thalassemia Trait
The beta thalassemia trait, also known as beta thalassemia minor, is an inherited blood condition that occurs when a person receives one mutated beta-globin gene from one parent and one normal gene from the other parent. Individuals with this condition are considered carriers of thalassemia rather than patients with severe disease. In most cases, people with the beta thalassemia trait lead healthy, active, and completely normal lives.
Hemoglobin is a vital protein inside red blood cells that carries oxygen throughout the body. The beta-globin gene helps produce an important part of hemoglobin. When one beta-globin gene is altered or mutated, the body may produce smaller red blood cells or slightly lower hemoglobin levels. However, because one normal gene is still functioning properly, the body can usually maintain adequate oxygen transport without major complications.
Many people discover they have the beta thalassemia trait only after routine blood work shows mild anemia or unusually small red blood cells. Others may learn about it during premarital screening, pregnancy testing, or family genetic evaluations. Understanding your carrier status is extremely important because it can affect future generations and family planning decisions.
The beta thalassemia trait is especially common in regions such as the Mediterranean, the Middle East, South Asia, Southeast Asia, and parts of Africa. Due to migration and global population movement, the condition is now found worldwide.
How Genetics Play a Role
Genetics are the primary cause of the beta thalassemia trait. Every individual inherits two beta-globin genes, one from each parent. If only one gene contains a mutation, the person becomes a carrier and develops beta thalassemia minor. If both inherited genes are severely affected, the individual may develop beta thalassemia major, which is a much more serious blood disorder requiring lifelong medical care.
According to the Centers for Disease Control and Prevention, thalassemia is inherited in an autosomal recessive pattern. This means both parents must pass on affected genes for a child to develop the severe form of the disease.
When two carriers of the beta thalassemia trait have children together, each pregnancy carries:
- A 25% chance the child will inherit beta thalassemia major
- A 50% chance the child will inherit the beta thalassemia trait
- A 25% chance the child will inherit completely normal beta-globin genes
Because of these inherited risks, genetic counseling and carrier testing are strongly encouraged before marriage or pregnancy, especially in communities where thalassemia is common. Early screening helps couples make informed decisions about family planning and future healthcare needs.
Modern testing methods such as hemoglobin electrophoresis, complete blood count (CBC), and DNA analysis can accurately identify whether someone carries the beta thalassemia trait. In many countries, screening programs have significantly reduced the number of severe thalassemia births through education and early detection.
How Genetics Play a Role
Genetics are the foundation of the beta thalassemia trait. Every person inherits two beta-globin genes, one from each parent. These genes are responsible for helping the body produce beta-globin chains, an essential component of hemoglobin. Hemoglobin allows red blood cells to carry oxygen from the lungs to tissues throughout the body.
When one beta-globin gene contains a mutation and the other remains normal, the person develops the beta thalassemia trait, also called beta thalassemia minor. In this situation, the body can still produce enough healthy hemoglobin to function normally, although red blood cells may become smaller and mild anemia can sometimes occur.
According to the Centers for Disease Control and Prevention, beta thalassemia is inherited through an autosomal recessive pattern. You can learn more about inherited thalassemia conditions through CDC Thalassemia Information.
The beta thalassemia trait is especially common among people with Mediterranean, Middle Eastern, African, and Southeast Asian ancestry. In countries where thalassemia is more widespread, community screening programs and genetic testing are often encouraged before marriage or pregnancy.
If both parents carry the beta thalassemia trait, each pregnancy carries:
- A 25% chance the child will inherit beta thalassemia major
- A 50% chance the child will inherit the beta thalassemia trait
- A 25% chance the child will inherit normal beta-globin genes
Beta thalassemia major is a severe blood disorder that may require lifelong blood transfusions and ongoing medical treatment. Because of this risk, doctors often recommend genetic counseling for couples who may be carriers.
The World Health Organization also highlights the importance of early screening and public awareness for inherited blood disorders. Additional educational resources are available through WHO Genetic Disorders Information.
Modern medical testing can accurately identify carrier status through:
- Complete Blood Count (CBC)
- Hemoglobin electrophoresis
- DNA and genetic testing
- Iron studies to rule out iron deficiency anemia
Early testing plays a major role in family planning and healthcare awareness. Many people discover they carry the beta thalassemia trait during routine blood work, pregnancy screening, or family medical evaluations. Knowing your carrier status allows families to make informed medical and reproductive decisions while helping reduce the risk of severe thalassemia conditions in future generations.
What is the Beta Thalassemia Trait?
To grasp the importance of carrier testing, you must first understand how hemoglobin works. Hemoglobin is the complex protein inside your red blood cells responsible for transporting oxygen from your lungs to your tissues. This protein relies on a delicate balance of alpha-globin and beta-globin chains.
A person with the beta thalassemia trait has inherited one altered beta-globin gene from one parent and one normal gene from the other. This single genetic change creates a carrier status. The body still produces enough normal hemoglobin to function well, but the red blood cells might be slightly smaller or paler than average.
Because the body compensates effectively, most carriers live entirely normal lives. They do not have a disease. However, they carry the genetic potential to pass this altered gene to the next generation.
The Crucial Role of Carrier Testing
Testing is one of the most effective strategies for identifying the beta thalassemia trait early. Because carriers remain largely asymptomatic, many individuals are completely unaware of their genetic status until they actively look for it.
Testing becomes exceptionally important before marriage, pregnancy, or starting a family. If both partners carry the beta thalassemia trait, there is a 25 percent chance with every pregnancy of having a child with beta thalassemia major. This is a severe, lifelong blood disorder that requires intensive medical intervention. Early awareness allows couples to explore genetic counseling, prenatal testing, and informed family planning options.
Medical professionals strongly recommend screening for specific groups of people:
- Individuals with a known family history of thalassemia or other different kinds of blood diseases.
- Couples actively planning to have children.
- People experiencing unexplained, mild anemia that does not respond to dietary changes.
- Individuals from high-risk ethnic backgrounds, particularly those of Mediterranean, Middle Eastern, South Asian, and Southeast Asian descent.
- Pregnant women during their early prenatal care appointments.
Distinguishing Between the Trait and Major Disease
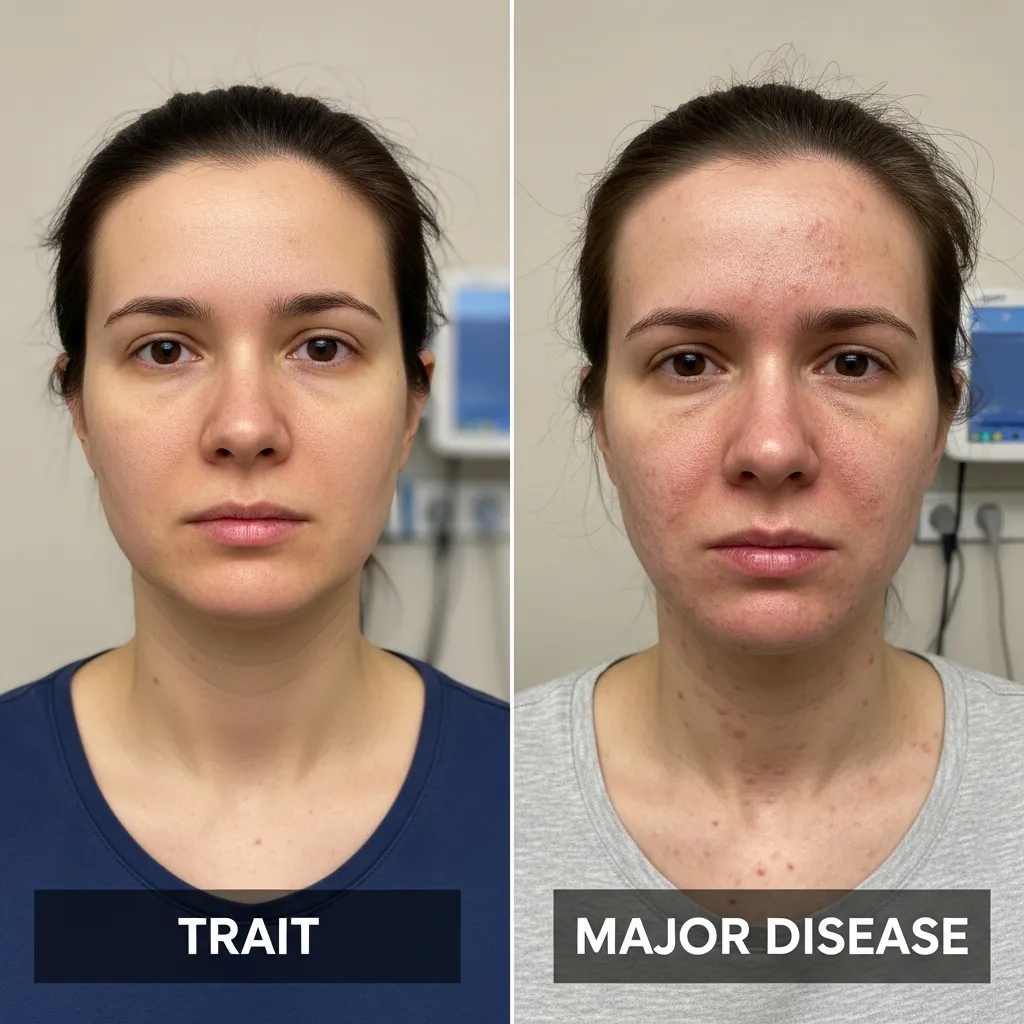 A common source of anxiety for newly diagnosed carriers is confusing the beta thalassemia trait with beta thalassemia major. These are two vastly different medical situations.
A common source of anxiety for newly diagnosed carriers is confusing the beta thalassemia trait with beta thalassemia major. These are two vastly different medical situations.
Beta thalassemia trait is strictly a carrier condition. You possess only one affected gene. Symptoms are usually mild or completely absent, and you do not require complex medical treatments.
Beta thalassemia major occurs when a child inherits two severely affected beta-globin genes—one from each parent. This condition halts normal hemoglobin production almost completely. Patients face severe anemia, delayed childhood growth, profound fatigue, and serious skeletal changes. For instance, severe marrow expansion can cause facial bone deformities, often referred to medically as the thalassemia chipmunk face. Managing beta thalassemia major requires lifelong blood transfusions and ongoing iron chelation therapy to survive.
Understanding this difference reduces fear and highlights exactly why genetic screening before pregnancy is so valuable. With modern medical care, the beta thalassemia life span for major cases has improved drastically, but preventing the disease through carrier awareness remains the best approach.
How Doctors Diagnose the Condition
Diagnosing the beta thalassemia trait requires specific laboratory tests. A standard blood test alone cannot always provide the full picture.
Common tests used to identify this trait include:
- Complete Blood Count (CBC): This measures the size, number, and maturity of your red blood cells. Carriers often have a high number of very small red blood cells.
- Hemoglobin Electrophoresis: Also known as a hemoglobin panel, this specialized test separates the different types of hemoglobin in your blood. It is the gold standard for identifying abnormalities. You can learn more through this comprehensive hemoglobin panel test guide.
- Genetic Testing: DNA analysis confirms the exact genetic mutations present, leaving no room for doubt regarding your carrier status.
- Iron Studies: Doctors must distinguish the thalassemia trait from basic iron deficiency anemia, as the two conditions look incredibly similar under a microscope.
These tests ensure accurate diagnosis and prevent improper treatments.
Living With the Beta Thalassemia Trait
Receiving a carrier diagnosis does not mean your life has to change. Most individuals with the beta thalassemia trait live healthy, active lives without any major complications. The condition usually does not require special medical treatment, regular blood transfusions, or restrictive lifestyle changes.
However, maintaining your overall health remains important. Eating a nutrient-rich diet, staying physically active, and attending routine medical checkups support your long-term well-being. Doctors may occasionally monitor your blood levels to ensure any mild anemia symptoms remain stable.
You must avoid self-diagnosing iron deficiency. Because the red blood cells of a thalassemia carrier look small and pale, some patients are mistakenly treated for iron deficiency anemia even when their iron levels are perfectly normal. Taking iron supplements without a confirmed deficiency and medical supervision can lead to dangerous iron buildup in your organs, causing unnecessary health complications.
Navigating Pregnancy as a Carrier
Women carrying the beta thalassemia trait may require slightly closer monitoring during pregnancy. The natural increase in blood volume during gestation can make mild anemia more noticeable, leading to increased fatigue.
In most cases, pregnancy remains completely safe with proper prenatal care and medical supervision. Your obstetrician will monitor your hemoglobin levels closely and adjust your prenatal vitamins as needed. If you want to understand how a related trait impacts gestation, you can read about navigating an alpha thalassemia carrier pregnancy.
The Importance of Thalassemia Awareness
 Public awareness about the beta thalassemia trait serves as the strongest defense against severe inherited blood disorders. Knowledge empowers communities to take proactive steps regarding their genetic health.
Public awareness about the beta thalassemia trait serves as the strongest defense against severe inherited blood disorders. Knowledge empowers communities to take proactive steps regarding their genetic health.
Many countries with high prevalence rates now promote premarital screening programs, school education campaigns, and extensive family testing initiatives. These public health efforts vastly improve early diagnosis and prevention.
Effective educational programs encourage people to:
- Understand the mechanics of inherited blood disorders.
- Get tested long before marriage or pregnancy.
- Seek professional genetic counseling to understand personal risks.
- Support families actively affected by severe forms of the disease.
- Reduce the social stigma sometimes associated with carrying genetic conditions.
Greater awareness and routine early testing will continue to play a major role in improving healthcare outcomes worldwide. By normalizing carrier testing, we help future generations avoid the physical and emotional challenges of severe inherited blood disorders.
Frequently Asked Questions (FAQ)
1. What is the beta thalassemia trait?
The beta thalassemia trait, also called beta thalassemia minor, is an inherited blood condition where a person carries one mutated beta-globin gene and one normal gene. Carriers usually experience mild or no symptoms.
2. Is beta thalassemia trait dangerous?
In most cases, the beta thalassemia trait is not dangerous. Most carriers live healthy and normal lives without severe medical complications.
3. Can beta thalassemia trait cause anemia?
Yes, some carriers may develop mild anemia. Symptoms can include fatigue, weakness, or pale skin, but the condition is generally mild compared to beta thalassemia major.
4. How is beta thalassemia trait inherited?
The condition is inherited genetically from parents. A person develops the trait when they inherit one mutated beta-globin gene from either parent.
5. Can two carriers have a healthy child?
Yes. If both parents carry the beta thalassemia trait, there is:
- A 25% chance of a child with beta thalassemia major
- A 50% chance of a child with the carrier trait
- A 25% chance of a child without affected genes
6. How is beta thalassemia trait diagnosed?
Doctors usually diagnose the condition through blood tests such as:
- Complete Blood Count (CBC)
- Hemoglobin electrophoresis
- Genetic testing
- Iron studies
7. Is beta thalassemia trait the same as iron deficiency anemia?
No. Although both conditions can appear similar on blood tests, beta thalassemia trait is a genetic disorder while iron deficiency anemia results from low iron levels.
8. Do carriers need treatment?
Most people with the beta thalassemia trait do not require special treatment. Regular health monitoring and accurate diagnosis are usually sufficient.
9. Why is carrier screening important?
Carrier screening helps individuals and couples understand genetic risks before having children. Early testing can help prevent severe thalassemia conditions in future generations.
10. Can people with beta thalassemia trait live normal lives?
Yes. Most carriers live completely normal lives, including having careers, exercising, and raising healthy families without major health restrictions.
Conclusion
Understanding the beta thalassemia trait is important for personal health awareness, accurate diagnosis, and informed family planning. Although most carriers experience few or no symptoms, knowing your carrier status can help prevent serious inherited blood disorders in future generations. Early testing, genetic counseling, and proper medical guidance allow individuals and families to make confident healthcare decisions. By increasing awareness about beta thalassemia trait, more people can access early screening, reduce complications, and better protect their family’s long-term health.
 A common source of anxiety for newly diagnosed carriers is confusing the beta thalassemia trait with beta thalassemia major. These are two vastly different medical situations.
A common source of anxiety for newly diagnosed carriers is confusing the beta thalassemia trait with beta thalassemia major. These are two vastly different medical situations. Public awareness about the beta thalassemia trait serves as the strongest defense against severe inherited blood disorders. Knowledge empowers communities to take proactive steps regarding their genetic health.
Public awareness about the beta thalassemia trait serves as the strongest defense against severe inherited blood disorders. Knowledge empowers communities to take proactive steps regarding their genetic health.